Influenza (FLU) Update for Week Ending 11-30-19
Influenza (FLU) Update for Week #48 — Week Ending 11-30-19
The CDC reported that seasonal flu activity continued to increase over the previous week; from a national perspective, ILI has been at/above baseline for four weeks, and many areas of the country have significant levels of flu, while some areas are still seeing only low levels of flu activity. According to the data, the 2019/20 flu season is ramping up earlier and faster when compared with other recent years (see chart below). The one exception is the 2009/10 season, displayed on the chart with a silver line, which represents the pandemic flu year. Most of the current flu activity is caused by Influenza B/Victoria when usually occurs toward the end of the flu season; A(H1N1) is the next most common, followed by A(H3N2), which has decreased in percentage of positive flu tests. Influenza-like illness (ILI) is defined as a temperature at/above 100o F [37.8o C] and cough and/or sore throat without a known cause other than flu. A Flu case, that is included in CDC data, indicates a positive flu test read by either a Clinical or Public Health Lab.
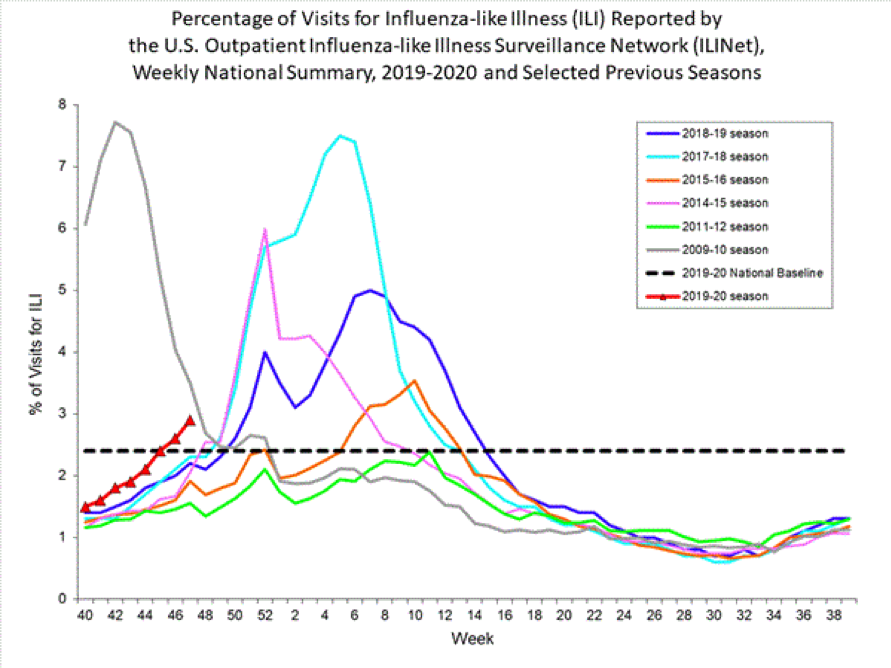
Chart copied from the CDC URL https://www.cdc.gov/flu/weekly/index.htm ; content source Center for Disease Control and Prevention, National Center for Immunization and Respiratory Diseases (NCIRD); page last reviewed 12/6/19; chart accessed 12/7/19.
Diagnosed Flu and ILI are expected to continue to increase over the next few weeks and flu activity is likely to persist for several more months. It is recommended by public health officials & health care providers that for all those 6 months or older, flu vaccinations should be completed ASAP unless they have a valid medical contraindication. Most will receive a vaccination that covers 4 strains of influenza.
The severity of Flu & ILI for this season, as well as which viruses will ultimately dominate, is still too early to identify, but there are hints that this season may be more severe than many, since most recent seasons have hit the national threshold for ILI typically between weeks #48 and #50, but this season hit the threshold at week #45 and has continued to climb. As more data is collected by the CDC further into the season, its severity and other report components will be included in this Summary.
See this link for more details, including charts, graphs, and maps: https://www.cdc.gov/flu/weekly/index.htm
FirstWatch RIN (Reginal Influenza Network) Alerts increased significantly over previous weeks.
For the most recently reported week ending November 30, 2019, the CDC reported:
–ILI visits to clinics and other non-hospital facilities was at 3.5%, higher than last week’s 2.9% and above the national baseline of 2.4%. The regional range was between 1.8% and 6.9% (up only 0.1%) for Week #48. Nine of ten regions reported that outpatient visits for ILI were at/above their own regional baselines. Only one region, Region 1 (CT, ME, MA, NH, RI, & VT), remained below their region-specific baseline for ILI.
–Flu cases, documented by positive flu tests from Clinical Labs, showed that 10.2% of respiratory specimens tested for influenza were positive, which is higher than last week’s report of 8.0%.
— For this reporting period, viewed from a national standpoint, Influenza B/Victoria viruses were reported more frequently, then Influenza A(H1N1)pdm09 and Influenza A(H3N2) viruses, but are considered to be cocirculating. The predominant strain varied by region and patient age. To access specific state and regional information on circulating flu viruses, please see: https://gis.cdc.gov/grasp/fluview/fluportaldashboard.html
—Clinical Labs, which test many specimens to determine whether flu cases are increasing, decreasing, or staying stable, as well as a simple breakdown of A and B flu percentages, reported that positive flu specimens equaled 10.2% with 71.1% Influenza B and 28.9% Influenza A.
—Public Health Labs reported data which has a more limited number of specimens but provides a more specific breakdown of specific flu virus strains. Influenza B was detected at 62.2% and Influenza A at 37.8%. Further breakdown revealed that Influenza B showed 97.1% Victoria lineage and 2.9% Yamagata, while H1N1 is the dominant A with 79.2% and H3N2 at 20.8%. Influenza B viruses are typically seen in greater numbers nearer the end of the flu season rather than the beginning and may be a tougher flu for children.
–Vaccine Coverage: Testing of Influenza A(H1N1) samples revealed that all samples tested were well matched with the components in the 2019-20 flu vaccine, while 87.5% A(H3N2) Influenza virus samples matched; only 62.5% B/Victoria virus samples were a similarly matched. Testing of B/Yamagata samples were still pending at the time of the CDC’s report.
The CDC provides an interactive U.S. map that will link to each state’s public health authorities, ILI and Flu information and processes, as well as other diseases and public health topics. This site includes a tremendous amount of information at the State, and even Local, level.
Find it at this site: https://www.cdc.gov/flu/weekly/usmap.htm
—For Influenza-Like Illness (ILI)
High ILI Activity (Puerto Rico & 12 states): Alabama, Georgia, Louisiana, Minnesota, Mississippi, Nebraska, Nevada, New Mexico, South Carolina, Tennessee, Texas, and Washington
Moderate ILI Activity (New York City & 14 states): Arizona, Arkansas, Colorado, Connecticut, Florida, Hawaii, Kentucky, Maryland, Missouri, New Jersey, North Dakota, Oklahoma, Utah, and Virginia
Low Activity (Washington D.C. & 8 states): California, Illinois, Massachusetts, New York, North Carolina, Oregon, Pennsylvania, and Wisconsin
Minimal Activity (16 states): Alaska, Delaware, Idaho, Indiana, Iowa, Kansas, Maine, Michigan, Montana, New Hampshire, Ohio, Rhode Island, South Dakota, Vermont, West Virginia, and Wyoming
Insufficient Data to Calculate: U.S. Virgin Islands &
—For Flu (positive Flu tests)
Widespread Activity (16 states): Alabama, California, Connecticut, Georgia, Indiana, Louisiana, Massachusetts, Mississippi, Nevada, New Mexico, New York, Pennsylvania, South Carolina, Tennessee, Texas, and Virginia
Regional Activity (Puerto Rico & 14 states): Alaska, Arizona, Colorado, Florida, Idaho, Kentucky, Minnesota, Montana, Nebraska, Oklahoma, Oregon, Utah, Washington, and Wisconsin
Local Activity (17 states): Arkansas, Delaware, Hawaii, Illinois, Iowa, Maine, Maryland, Michigan, Missouri, New Hampshire, New Jersey, North Carolina, North Dakota, Ohio, South Dakota, Vermont, and Wyoming
Sporadic Activity (Washington D.C., U.S. Virgin Islands, & 3 states): Kansas, Rhode Island, and West Virginia
No Report: Guam
—Other Data:
Hospitalizations from Flu: There were a total of 784 lab-confirmed influenza-related cases that were hospitalized reported between 10/1/19 and 11/30/19. The hospitalization rate for all ages increased to 2.7 per 100,000 and is typical for this time period when compared with previous seasons. The highest rate was in those aged > 65 years (7.0/100,000), then children ages 0-4 (4.6/100,000), and then adults ages 50-64 (2.7/100,000). The vast majority were from infections with influenza A (57.5%), 41.5% with influenza B, 0.5% with both influenza A and B co-infection, and 0.5% which did not have a flu type determined. For the influenza A positives that had subtyping performed, 60.6% were A(H1N1) and 39.4% were A(H3N2).
Death rates for pneumonia & influenza in adults: from data as of 12/5/19, 4.8% of adult deaths during week #47 (ending 11/23) were associated with influenza and pneumonia. This is below the epidemic threshold of 6.4% for that week. This data reporting typically lags a week or more behind the reporting week.
One (1) pediatric death associated with influenza was reported during week #48, making a total of six (6) flu-associated pediatric deaths for the 2019-20 Flu Season.
International:
Canada:
Flu in Canada for Week #48 (11/23 – 11/30, 2019):
According to the Public Health Agency of Canada (PHAC), influenza activity increased again as is typical for this time period. The seasonal influenza season began last week, during Week #47. Influenza A(H3N2) continued to be the most common flu virus circulating, although A(H1N1) accounted for 40% of Influenza A positive specimens. Influenza B accounted for about 30% of all the positive specimens, which is atypical for this early in the season. All 53 Regions reported.
Localized Activity: in 6 Regions (11%): Ontario (2), Manitoba (1), Alberta (3)
Sporadic Activity: in 27 Regions (51%): Newfoundland & Labrador (1), Prince Edward Island (1), New Brunswick (2), Quebec (6), Ontario (5), Manitoba (3), Saskatchewan (2), Alberta (2), British Columbia (5)
No Activity: in 20 Regions (38%): Newfoundland & Labrador (3), Nova Scotia (4), New Brunswick (5), Manitoba (1), Saskatchewan (1), Yukon Territory (1) Northwest Territory (2), Nunavut (3)
PHAC Flu Watch Summary & Influenza/ILI Activity Map for Week #48 see: https://www.canada.ca/en/public-health/services/publications/diseases-conditions/fluwatch/2019-2020/week-48-november-24-30-2019.html
PHAC Home Page for Surveillance on Flu: https://www.phac-aspc.gc.ca/fluwatch/
Public Health Agency of Canada (PHAC) Home Page for Information on Flu:
https://www.canada.ca/en/public-health/services/diseases/flu-influenza.html
PHAC Provides Flu Watch Summary & Link to Full Influenza Reports Past & Present:
https://www.canada.ca/en/public-health/services/diseases/flu-influenza/influenza-surveillance/weekly-influenza-reports.html
PHAC Interactive Map for Flu Activity Across Canada:
https://www.canada.ca/en/public-health/services/diseases/flu-influenza/influenza-surveillance/map-activity-levels.html
PHAC Site that Explains How to Become a Canadian Flu Watcher:
https://www.canada.ca/en/public-health/services/diseases/flu-influenza/fluwatcher.html
Europe:
European Center for Disease Prevention & Control – Flu for Week #48 (11/25 – 12/1, 2019):
Influenza activity increased in some parts of Europe and more countries reported widespread or regional flu activity, although most still reported rates at or below baseline. For the second week in a row, specimens tested positive for flu for those going to sentinel PCPs for ILI and ARI at greater than 10%; this marks the beginning of the flu season in Europe. Flu viruses A & B, were found in specimens from those with respiratory illness seeking medical care, with more A flu dominant, but with influenza B reported dominant by four countries. Data from 21 countries/regions reported mortality from all causes were at expected levels for this time of year.
For more info see: https://flunewseurope.org/
Public Health England Flu Summary:
https://www.gov.uk/government/statistics/weekly-national-flu-reports
Global:
World Health Organization (WHO) Weekly Flu Summary (FluNet):
https://www.who.int/influenza/gisrs_laboratory/flunet/en/
WHO Global Flu Overview with Map and Text:
https://www.who.int/influenza/surveillance_monitoring/updates/latest_update_GIP_surveillance/en/
Global Epidemiology Reports:
WHO Collaborating Centers for Flu in Australia, Japan, & the United Kingdom
First Responder Specific Information
There are many websites that may be helpful in planning and managing seasonal flu within First Responder organizations. A few of those websites are included here:
NIOSH on Flu for Employers/Employees:
https://www.cdc.gov/niosh/topics/flu/
NIOSH Listing on Absenteeism in the Workplace throughout the US:
https://www.cdc.gov/niosh/topics/absences/default.html
Protection from Flu:
https://www.cdc.gov/flu/protect/habits/index.htm
World Map Showing Flu & Other Infectious Diseases:
https://www.healthmap.org/en/
- First Responders should be vaccinated for Flu each season to prevent getting flu themselves, taking it home to family members or transmitting it to patients in their care. Family members and patients may be at increased risk of complications from flu.
- Perform proper hand hygiene including frequent handwashing with soap and water, and the use of hand sanitizers in general, and particularly when providing patient care or after touching surfaces.
- Masks (N95 or 100) should be used in the presence of patients with cough and/or fever. Procedure or surgical masks can also be used but may not provide the same level of protection.
- Care should be taken to avoid touching their own face and mucous membranes (eyes, mouth, nose) since the flu virus is frequently found on surfaces such as door knobs, cot and equipment handles, phones, as well as clothing, bed clothes, etc. Once picked up on the hands from touching inanimate objects or from the secretions of a patient, it can transmit the flu (or any respiratory infection virus) via the mucous membranes of the face and head.
- Report signs/symptoms of flu to your physician or other appropriate provider for early assessment and care. Signs & symptoms suggest a period of contagiousness and out your patients and co-workers at risk.
- Cough and sneeze into your sleeve, if a tissue is not available, and not onto your hands.
- Stay away from others if you are sick.
- Be aware of your exposure risk and history. Take extra precautions or avoid those with immunocompromise, when possible, if you have a known or likely exposure.
- Antivirals may be indicated for the treatment of flu, particularly for those in high risk groups, those who are hospitalized or have severe, complicated or progressing flu. Those that present with 48 hours of the onset of symptoms may also be given antivirals, based on PCP judgement but make sure the practitioner is aware of their Frist Responder Role. See https://www.cdc.gov/flu/antivirals/whatyoushould.htm
- Flu is much more worrisome for the very young and the very old. Signs of ILI in this group requires careful assessment to rule out complications and these groups are much more likely to need to be transported to assure adequate care. Young children and those over 65 are typically at greater risk for complications, hospitalization, and even death. Hospitalization rates may also be elevated in those aged 50-64. Consideration should perhaps be given to monitoring these groups more closely, with inclination for more comprehensive assessment and transport for further evaluation, when presented with possible flu and any signs of complications.
Complications of flu, sometimes requiring hospitalization and even leading to death, tend to occur after the person has begun to get better from the flu and then appears to relapse. EMS personnel may want to look more closely at those patients when the call is not about the initial signs and symptoms of flu, but about increasing or different signs that have appeared.
- A study was published by the Institute for Clinical Evaluative Sciences in NEJM:

Image courtesy of ICES/PHO “The researchers add that patients should not delay medical evaluation for heart symptoms particularly within the first week of an acute respiratory infection.” (Lisa Schnirring, News Editor: CIDRAP News; Jan 25, 2018)
For more information on the Influenza and Heart Attack Study, please see the link below.
https://www.eurekalert.org/pub_releases/2018-01/pho-rcl011818.php

